Diabetes Canada is proud to be a leading supporter of diabetes research in Canada. Since 1975, we’ve supported outstanding diabetes research in Canada and provided more than $160 million in research grants, awards and partnerships to scientists across the country.
Since the discovery of insulin in Toronto in 1921, Canadian researchers have made huge strides and key advances in understanding diabetes. This is why, each year, we choose to fund Canada’s most renowned researchers in their quest for new and innovative developments in the prevention, treatment, management and cure for diabetes. The research is diverse in scope, covering a broad range of specialties and topics, and the underlying goal of each study remains the same—to create a world free of the effects of diabetes.
Through our funding opportunities, Diabetes Canada funds research to enhance our understanding of diabetes and its prevention, treatment, management, and cure. Diabetes Canada accepts funding proposals from all four pillars of health research, to ensure that we are funding the best in biomedical, clinical, health services, and/or population health research to improve the lives of people living with or at risk of diabetes and its complications.
Currently Funded Research
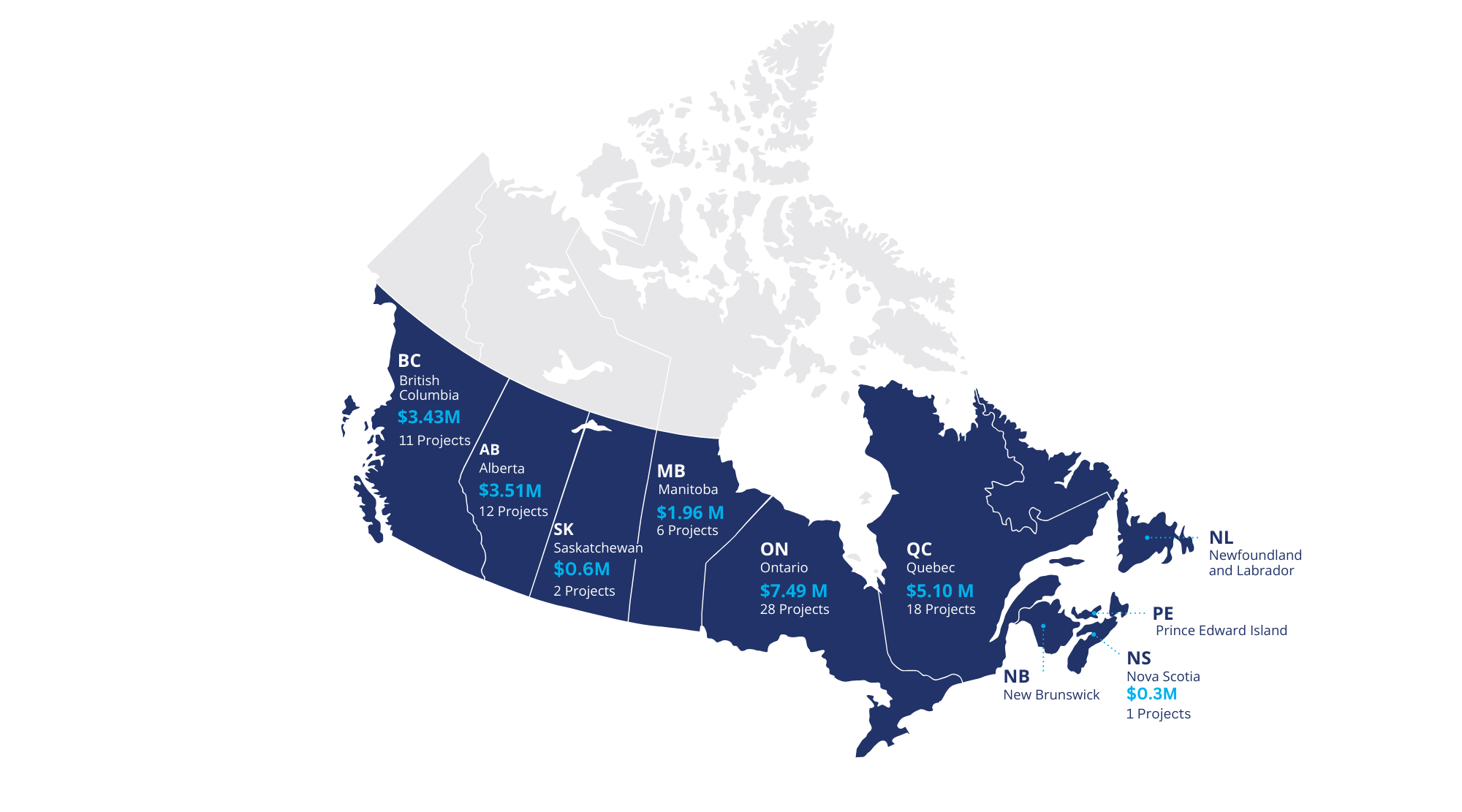
As of January 2024, Diabetes Canada is funding over 75 diabetes research projects involving over 260 researchers at 20 different research institutions across the country,
Current Research Funding Across Canada
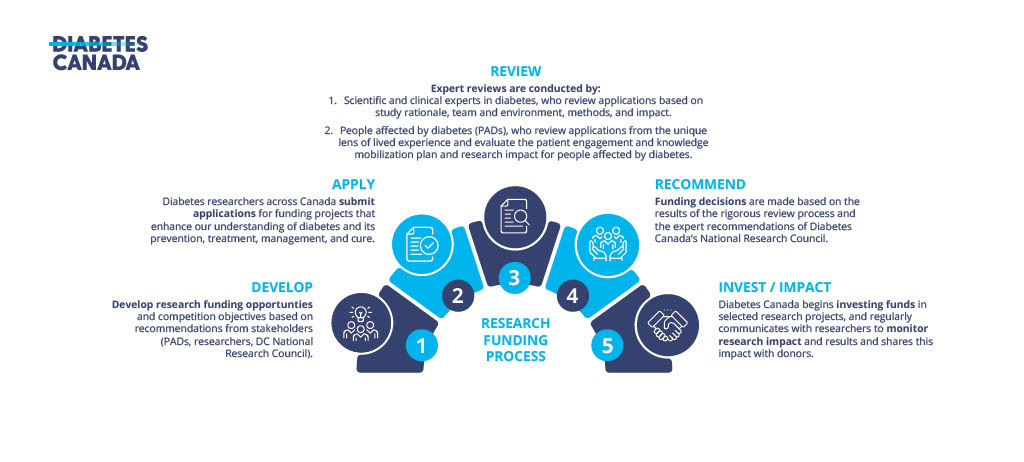
Research Funding Process
Investing for Impact: Diabetes Canada’s research funding process
Research Areas
Diabetes Canada funds research covering an array of topics to ensure that we are funding the best in biomedical, clinical, health services, and/or population health research to improve the lives of people living with or at risk of diabetes and its complications.
Causes
What happens in the body at the smallest levels that leads to the development of diabetes? What risk factors for diabetes exist in different populations? How is the risk of developing diabetes assessed?
Complications
Why do diabetes-related complications develop? How can they be prevented, delayed, or treated? What impact can the severity or treatment of diabetes have on other health conditions?
Cure
What will bring us closer to a cure for diabetes? Is there a way for diabetes to be reversed? What will a cure look like for all types of diabetes?
Prevention
How can the risk of developing diabetes be reduced? How can diabetes be prevented, or its onset delayed? What prevention methods are effective for more at-risk populations?
Screening
How do we effectively assess the risk factors for the development of diabetes? Are there better ways to support early detection? What screening guidelines should different populations follow?
Treatment
Are there better ways to treat diabetes? How can we minimize negative side effects? How can we identify and eliminate barriers to accessing treatment?
Research Pillars
Research can be broken down into four big categories. The Canadian Institutes of Health Research (CIHR) defines these categories as “pillars”. Each pillar interacts with the others to create a pipeline of research that goes from labs and test tubes to medications and treatments that can be used by people living with diabetes.
Pillar 1: Biomedical research
Involves studying molecules, cells and tissues to find out, at the microscopic level, how our bodies work in health and disease. Takes about 10 to 40 years before it impacts people with diabetes.
Pillar 2: Clinical research
Involves studying people, taking that information and turning it into treatments, diagnostic tests and cures. Takes five to 15 years before it impacts people with diabetes.
Pillar 3: Health services research
Involves measuring how treatments are being delivered to the population and whether they provide the promised benefit. Takes one to five years before delivering results that can be used to develop policy. How and when it impacts people with diabetes depends on governments implementing the findings.
Pillar 4: Population & public health
Involves studying the health of whole populations and subgroups within those populations, in particular, finding out if everyone is benefiting equally from advances in health services. Takes one to five years before delivering results that can be used to develop policy, and also depends on government action.
IDEA, Sex and Gender-Based and Race and Ethnicity-Based Analysis in Research
Diabetes Canada is committed to advancing inclusion, diversity, equity, and accessibility (IDEA) in health research. Inclusion is defined as the practice of ensuring that all individuals are valued and respected for their contributions and are equally supported. Diversity is defined as differences in race, colour, place of origin, religion, immigrant and newcomer status, ethnic origin, ability, sex, sexual orientation, gender identity, gender expression and age. Equity is defined as the removal of systemic barriers and biases, enabling all individuals to have equal opportunity to access and benefit from the research, as well as engage and participate in the research. Accessibility is defined as when the needs of all people are specifically considered, and products, services, and facilities are built so that they can be used by people of all abilities and demographics.
Sex and Gender-Based and Race and Ethnicity-Based Analysis and Reporting acknowledges and examines the biological and social differences that can affect the risk of developing certain diseases, individual response to medical treatments, accessing health-related resources and care, and impact quality of life and daily activities. Integrating this analysis into research design and practices has the potential to create more rigorous and inclusive health research that is more applicable and accessible to everyone.